Comment:
This is a study I go back to again and again as it’s well designed and demonstrates how important quality sleep is not just for quality of life, but for a significant improvement in overall survival.
We have many tools to help with sleep, including reminding people of the importance of it. This study highlights that it should be a strong focus for all cancer patients.
The Wonk Debate – Audio Critique & Clinical Commentary:
Summary:
Clinical Bottom Line
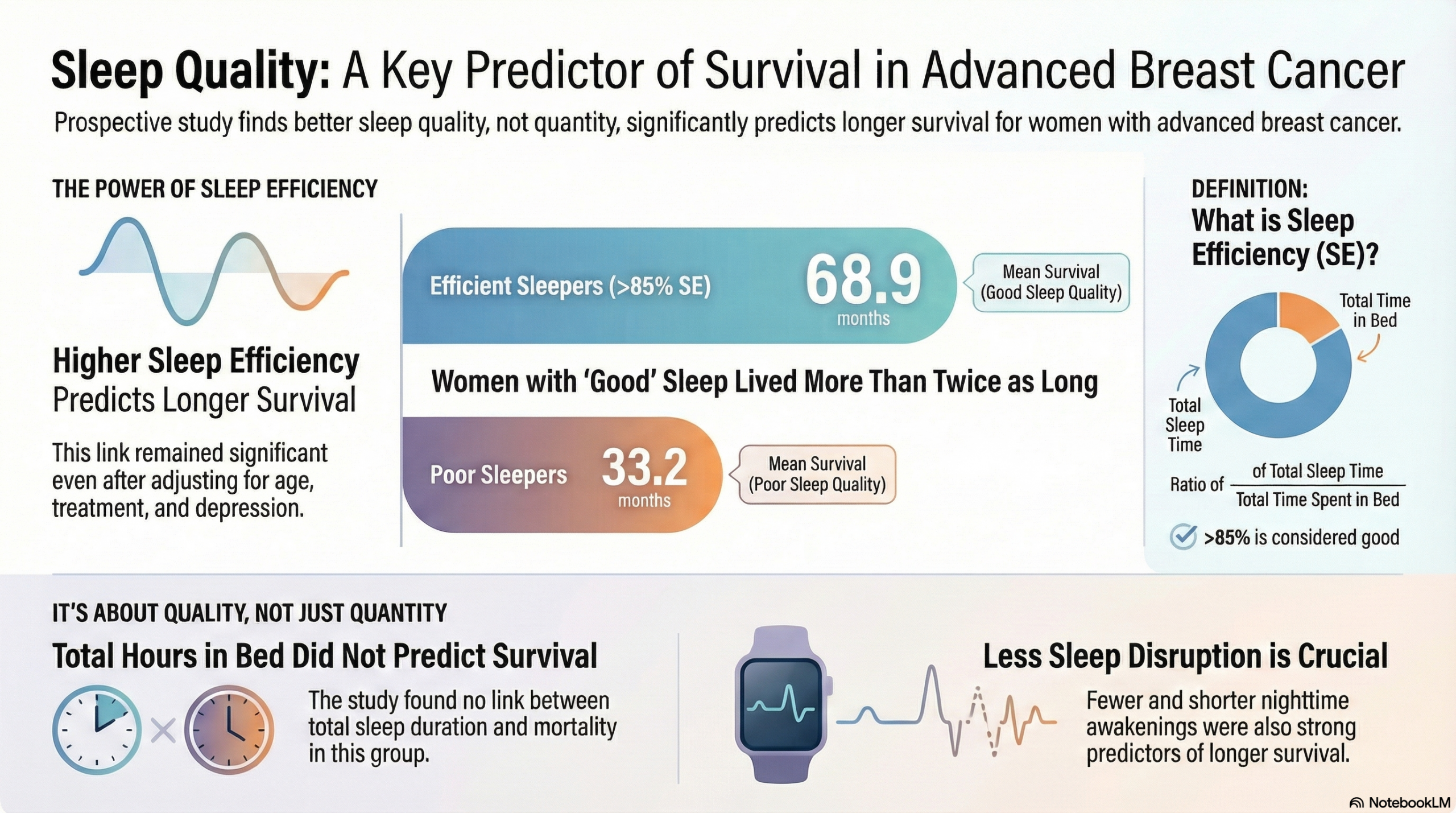
This prospective cohort study identifies objective Sleep Efficiency (SE) as a robust, independent prognostic factor for overall survival in women with advanced breast cancer. The data indicates that sleep quality (efficiency and consolidation) is significantly associated with survival, whereas sleep quantity (duration) is not. While the authors report that a 10% increase in SE is associated with a 32% reduction in mortality hazard, this is an observational finding. It implies a strong association potentially linked to circadian or immune dysregulation but cannot confirm that therapeutically improving sleep will causally extend life without further interventional trials.
Results in Context
Primary Outcome: Overall Survival & Sleep Efficiency
- Main Finding: Higher sleep efficiency was significantly associated with lower mortality over the 6-year follow-up period.
- Statistical Result: The Hazard Ratio (HR) was 0.96 (95% CI, 0.94–0.98; P < 0.001). This implies that for every 1% increase in sleep efficiency, the hazard of death decreased by approximately 4%.
- Clinical Cutoff (85%): Using the clinical standard of 85% efficiency, the difference in survival was marked. Women with “efficient” sleep (SE ≥ 85%) had a mean survival of 68.9 months, compared to only 33.2 months for those with poor sleep efficiency (SE < 85%).
Secondary Outcomes: Sleep Duration & Fragmentation
- Sleep Duration (Time in Bed): Notably, there was no significant association between shorter sleep duration (Time in Bed) and mortality (HR, 0.99; P = 0.09). The study highlights that quality appears to matter more than quantity in this population.
- Wake After Sleep Onset (WASO): Measures of sleep fragmentation were strong predictors. Lower WASO (minutes awake after initially falling asleep) was associated with significantly lower mortality (adjusted HR, 0.41; 95% CI, 0.25–0.67; P < 0.001).
- Wake Episodes: Fewer wake episodes and shorter duration of wake episodes were also independent predictors of lower mortality.
Assertive Critical Appraisal
Limitations & Bias (STROBE Framework)
- Risk of Reverse Causality: A primary concern in connecting sleep to cancer survival is whether patients slept poorly because they were closer to death (disease severity) or if poor sleep accelerated disease progression. The authors argue against “pre-terminal” sleep disruption driving the results by showing that survival curves continued to diverge over 6 years. However, without randomization, this cannot be fully ruled out.
- Confounding Control: The study adjusted for robust prognostic factors, including age, estrogen receptor status, metastatic spread (viscera vs. bone), depression, and cortisol levels. The persistence of the effect after these adjustments strengthens the validity of the association.
- Sample Characteristics: The sample (N = 97) was relatively small and demographically homogenous, consisting primarily of White women (86.6%) with high socioeconomic status and education. This limits the generalizability of the findings to more diverse populations or those with early-stage disease.
- Measurement Proxy: While actigraphy is an objective improvement over self-report, it is a proxy for sleep and not the gold standard of polysomnography.
Reporting Quality (STROBE)
The study provides clear inclusion/exclusion criteria and adequately describes the statistical handling of covariates. The distinction between the predictive value of sleep efficiency versus the lack of predictive value for sleep duration is clearly reported and clinically relevant.
Applicability
These findings are highly relevant for clinicians managing advanced breast cancer. They suggest that sleep disruption is not merely a quality-of-life issue but a potential survival risk factor. Screening for sleep efficiency (even via sleep diaries if actigraphy is unavailable) and treating insomnia may be a valuable adjunctive aspect of oncologic care.
Research Objective
To clarify the relationship between objective measures of sleep efficiency/disruption and survival among women with advanced breast cancer using a prospective design.
Study Design
- Design: Prospective Cohort Study.
- Methodology: Sleep was assessed at baseline using wrist-worn actigraphy and sleep diaries for 3 consecutive days. Survival was tracked over a median follow-up of 6 years.
- Analysis: Cox Proportional Hazards Models were used, adjusting for known prognostic factors (medical and demographic).
Setting and Participants
- Setting: Recruitment occurred through oncologists at Stanford University Medical Center and the greater San Francisco Bay area.
- Participants: 97 women (mean age 54.6 ± 9.8 years) with metastatic (74.2%) or locally advanced (18.6%) breast cancer.
- Key Exclusions: History of other active cancers, recent corticosteroid use, or major psychiatric illness.
Bibliographic Data
- Title: Actigraphy-Measured Sleep Disruption as a Predictor of Survival among Women with Advanced Breast Cancer
- Authors: Palesh O, Aldridge-Gerry A, Zeitzer JM, Koopman C, Neri E, Giese-Davis J, Jo B, Kraemer H, Nouriani B, Spiegel D
- Journal: SLEEP
- Year: 2014
- DOI: 10.5665/sleep.3642
Original Article:
Full text: PubMed Central
Fair Use & Copyright: This post provides a transformative, thesis‑driven critical appraisal intended for educational and scholarly purposes. It is not a reproduction of, nor a market substitute for, the original research article.
Support the Version of Record: To support the copyright holders and verify the underlying data—including primary survival curves, risk estimates, and other core outcomes—readers are strongly encouraged to access the original Version of Record via the link or DOI provided above.
Medical Disclaimer: This content is for informational and educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment.
