Comment:🩺
This study of 390 paired primary and metastatic breast cancers provides some of the most compelling institutional data to date, confirming the biological profile of a breast cancer can and often does change dramatically upon metastasis.
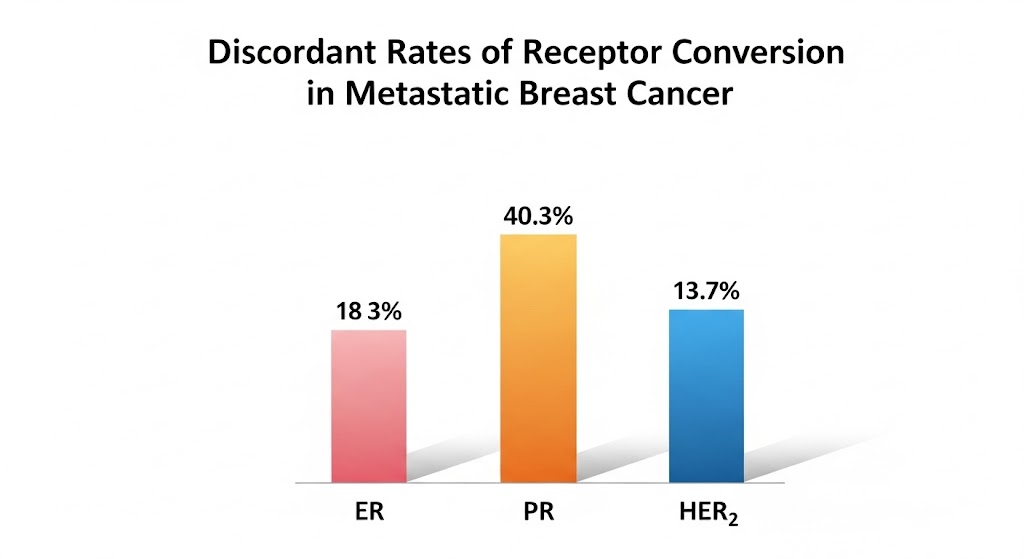
The sheer magnitude of the discordance rates—especially the 40.3% change for Progesterone Receptor (PR) and the 18.3% change for Estrogen Receptor (ER)—is a stark, mechanism-driven argument for adhering to current guidelines to re-biopsy of accessible metastatic sites.
Consider the practical implications:
-
Loss of Hormone Sensitivity: The majority of conversions were positive to negative for ER and PR. A patient whose primary tumor was ER-positive, and who subsequently loses that receptor in their metastasis, is highly unlikely to respond to further endocrine therapy. Continuing with tamoxifen or an aromatase inhibitor in this setting would represent ineffective treatment and unnecessary toxicity.
-
Missing a Targeted Opportunity: While less frequent, the conversion from HER2-negative to HER2-positive (a “gain” of the receptor) occurs in 8.1% of cases. Missing this gain means missing an opportunity to treat a patient with highly effective, life-prolonging HER2-targeted therapy (like trastuzumab or T-DM1).
Furthermore, the observation that discordance also occurs between different metastatic sites (e.g., bone vs. liver) complicates treatment selection even further, underscoring the genetic instability and heterogeneity of the disease.
The retrospective nature of the study prevents it from definitively proving the predictive value (i.e., that changing therapy based on the new receptor status improves outcomes), but the prognostic data is clear: the receptor status of the metastatic lesion is strongly associated with Overall Survival (OS).
From a prevention of recurrence focus, this means that it is likely that cancer cells that are in the system and looking to set up new sites are already a different receptor status, and therefore our clinical choices are more complex than we realized.
Summary:
Clinical Bottom Line
This large, single-institution retrospective study strongly suggests that receptor conversion (a change in Estrogen Receptor (ER), Progesterone Receptor (PR), or HER2 status) is a frequent event in the progression of breast cancer (BC) and can occur between the primary tumor and its metastases, as well as among different metastatic sites . The overall discordant rates were notable, especially for PR (40.3%), followed by ER (18.3%), and HER2 (13.7%) .
Crucially, the majority of conversions were from a positive to a negative status for all three receptors, which could be explained by the selective pressure of systemic therapy . The findings support the current practice guidelines that repeat biopsy and biomarker testing of accessible metastatic lesions are warranted to ensure appropriate targeted therapy is selected in the pursuit of precision medicine .
Results in Context
Main Results
The study examined 390 paired primary and metastatic breast carcinomas to determine the rate of receptor conversion, which is defined as the change (gain or loss) of hormone receptor or HER2 status between primary and metastatic tumors within the same patient .
-
Estrogen Receptor (ER): The overall discordant rate was 18.3% .
-
The conversion was significantly more frequent from positive to negative (loss of ER: 20.7%) compared to negative to positive (gain of ER: 10.9%) .
-
Semiquantitative analysis showed a significant 25% decrease in ER expression (H-score) in metastases compared to primary tumors .
-
-
Progesterone Receptor (PR): The overall discordant rate was the highest at 40.3% .
-
This rate was significantly higher than for both ER and HER2 .
-
Similar to ER, PR converted twice as frequently from positive to negative (loss of PR: 50%) than vice versa (gain of PR: 24.4%) .
-
There was an average 57% reduction of PR expression in metastatic tumors .
-
-
HER2: The overall discordant rate was 13.7% .
-
Conversion from positive to negative (loss of HER2: 28.7%) was significantly more common than from negative to positive (gain of HER2: 8.1%) .
-
Prognostic vs. Predictive Value
The study primarily evaluated the prognostic value of receptor conversion by analyzing its association with survival outcomes .
-
ER Status and Survival:
-
Metastasis-Free Survival (MFS): Any positive ER status (in primary or metastatic tumor: +/+, +/-, or -/+) was associated with a prolonged MFS compared with tumors that remained ER-negative in both primary and metastasis (-/-) .
-
Overall Survival (OS): A positive ER status in the metastatic tumor (regardless of primary: +/+ or -/+) was associated with a superior OS compared with the -/- ER status .
-
-
PR Status and Survival:
-
MFS: +/+ and +/- PR conversion were associated with a superior MFS when compared with -/- PR status .
-
OS: A negative PR status in the metastatic tumor (regardless of primary: +/- or -/-) was associated with a worse prognosis when compared with a PR-positive tumor without conversion (+/+) . This finding may reflect the role of PR as a surrogate for functional ER activation .
-
Specialized Outcomes
-
Discordance Among Metastatic Sites: In a subset of patients with multiple distant metastases, discordance in receptor status was observed between the different metastatic sites: ER (27.5%), PR (39.4%), and HER2 (14.3%) .
-
Site-Specific Discordance: A trend of higher PR discordance was seen in bone metastases when compared to other common organs of relapse, although it did not reach statistical significance .
Assertive Critical Appraisal
Appraisal of Biomarker Claim (Prognostic vs. Predictive)
The study successfully established the prognostic significance of receptor conversion, especially for ER and PR, by correlating the conversion status with Metastasis-Free and Overall Survival . The design—a retrospective analysis of a cohort with paired primary and metastatic tissue—is appropriate for assessing a prognostic association .
However, the study’s ability to demonstrate predictive value (i.e., whether changing therapy based on the metastatic receptor status results in better outcomes) is limited . The paper itself notes that all patients in the cohort received standard of care treatment at the time of diagnosis, and systemic therapy may have had a confounding effect on survival outcomes, which is an inherent limitation of this type of retrospective study . A large, prospective trial would be needed to definitively confirm the predictive value of retesting by documenting the outcome of patients whose systemic therapy decisions were actively changed based on the new metastatic receptor status .
Reporting Quality Assessment (REMARK)
The reporting quality is generally strong, particularly considering the retrospective nature of the cohort:
-
Patient Population: The study population (390 paired primary and metastatic cases) is clearly defined, and exclusions (locoregional recurrence, de novo metastatic BC) are explicitly stated .
-
Biomarker Assay Methodology: The methodology for receptor analysis is well-detailed, including the specific antibodies (clones 6F11, SP1, 1A6, 1E2, SP3, 4B5) used over time and the H-score semiquantitative analysis . The institutional efforts to minimize pre-analytical variables (e.g., non-decalcification of bone biopsies) is a strength .
-
Statistical Methods and Cut-points: The cutoff value for positivity (1% for ER/PR; 3+ or positive ISH for HER2) is stated, adhering to the current ASCO/CAP guidelines . The use of both categorical data analysis (chi-squared test) and continuous data analysis (H-score with Student’s t test) provides a robust assessment of receptor change .
Applicability
The findings are highly applicable to general clinical practice and are supportive of current guidelines . The high conversion rate, particularly the loss of PR and ER, has direct implications for metastatic breast cancer management, reinforcing the importance of re-biopsy and re-testing to guide endocrine and HER2-targeted therapy . The recognition of heterogeneity between different metastatic sites is a powerful finding that highlights the complexity of tumor biology and provides rationale for why targeted therapy may fail even in the metastatic setting .
Study Details
Research Objective 🔬
The study’s objective was to provide a large, single-center cohort analysis to assess the frequency of estrogen receptor (ER), progesterone receptor (PR), and human epidermal growth factor receptor-2 (HER2) conversion in metastatic breast cancer and analyze the association between receptor conversion and prognostic outcomes .
Study Design 📝
-
Study Design: This was a retrospective cohort study analyzing paired samples of primary and metastatic breast carcinomas .
-
Clinical Endpoints:
-
Primary Endpoints: Overall discordant rates for ER, PR, and HER2 .
-
Secondary Endpoints: Metastasis-free survival and overall survival, stratified by the four receptor conversion categories (+/+, +/-, -/+, -/-) .
-
Setting and Participants 🧑🤝🧑
-
Setting: The study used the Surgical Pathology database of a single academic institution (The University of Alabama Birmingham) .
-
Participants: A total of 390 paired primary and metastatic breast carcinomas from 348 patients were included. Patients were selected if they had matched primary and distant metastatic BC samples with receptor studies available between 1998 and 2019 .
-
Exclusions: Locoregional recurrence, de novo metastatic BCs, metastases to ipsilateral regional lymph nodes, and patients who did not receive systemic therapy were excluded . Bone biopsy specimens that required decalcification were avoided due to potential impact on receptor analysis .
Bibliographic Data
-
Title: Receptor conversion in metastatic breast cancer: analysis of 390 cases from a single institution
-
Authors: Rong Chen, Morad Qarmali, Gene P. Siegal, Shi Wei
-
Journal: Modern Pathology
-
Year: 2020
Original Article:
Full text: Here
