Comment:⚠️
This systematic review and meta-analysis consolidates the global data, providing moderate certainty evidence that the receptor status of a breast cancer is far from static. The findings confirm that the tumor we treat at the metastatic stage is often biologically different from the primary tumor excised years earlier.
The high conversion rates are not just interesting academic points; they represent significant, actionable changes that directly impact treatment:
-
Progesterone Receptor (PR) Loss is Extreme: With a staggering 49.4% of PR-positive primaries losing the receptor upon metastasis, basing endocrine therapy decisions solely on the primary tumor’s PR status is clearly insufficient. PR loss is often an early indicator of a less hormone-sensitive, more aggressive disease.
-
Missing a New Target: The 9.5% conversion rate from HER2-negative to HER2-positive may seem small, but in the context of metastatic disease, this represents a patient who could be immediately eligible for highly effective, life-prolonging HER2-targeted therapies. Relying on an old negative biopsy means we are missing a chance to improve survival.
-
Site Matters: The statistically significant differences in ER discordance based on the metastatic site (highest in bone and CNS) highlights the selective pressure of the microenvironment. This suggests that the tumor adapts differently in the brain versus the liver, demanding site-specific receptor information when possible.
In an era of personalized medicine, these results constitute a powerful reason to re-biopsy accessible metastatic lesions. Continuing therapy based on outdated receptor information risks both providing ineffective treatment (when receptors are lost) and withholding life-changing targeted therapy (when HER2 is gained).
From a recurrence prevention perspective, we must expand our thinking beyond the static information from the pathology of the original site.
Clinical Bottom Line
This meta-analysis provides Moderate certainty evidence confirming that receptor conversion for Estrogen Receptor alpha (ER), Progesterone Receptor (PR), and Human Epidermal growth factor Receptor 2 (HER2) occurs frequently in distant breast cancer metastases. This finding stresses the clinical importance of reassessing receptor status in metastatic tissue whenever possible to guide appropriate therapy, as treatment decisions are currently still largely based on the primary tumor’s characteristics.
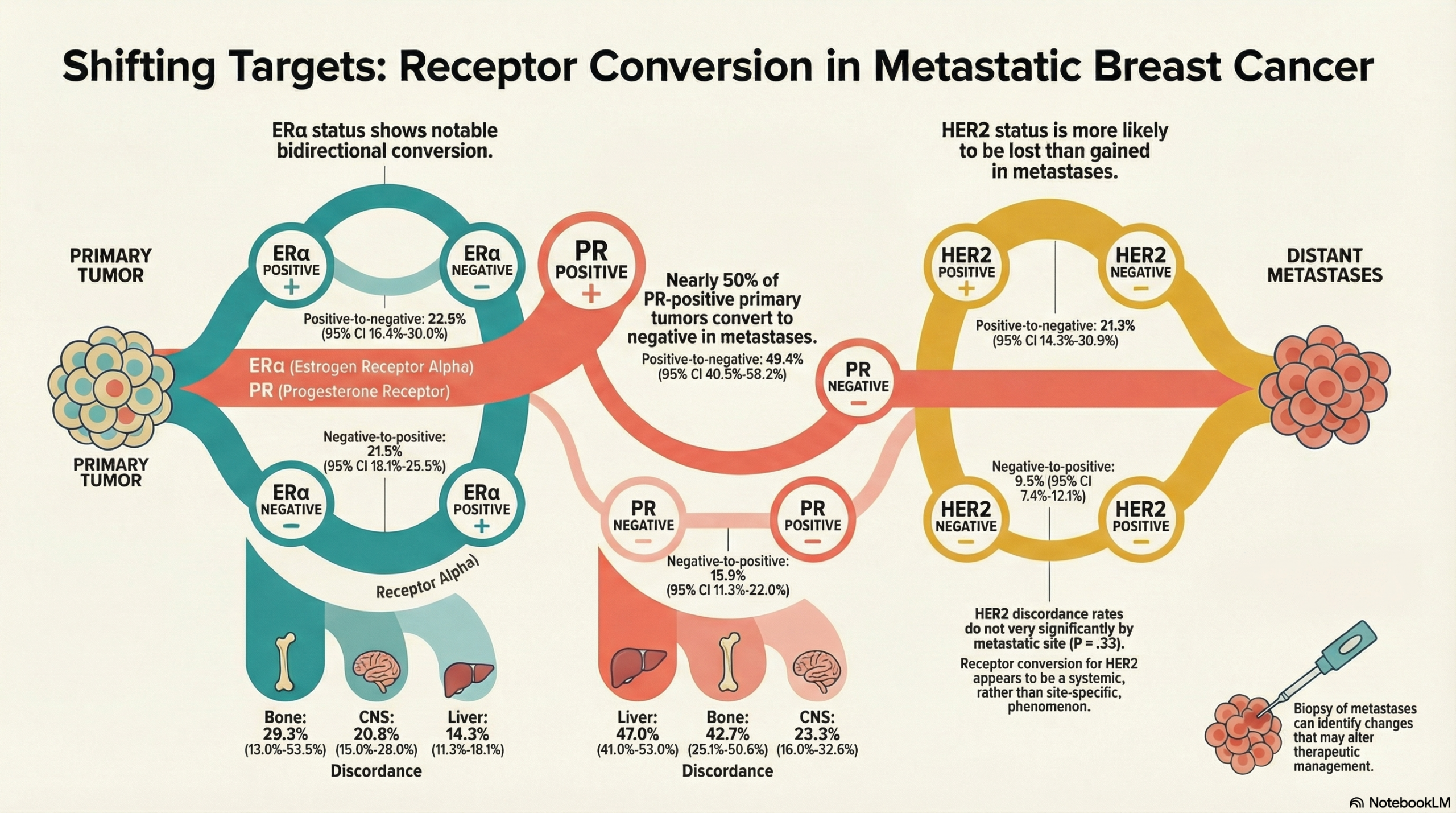
The pooled data show that PR and HER2 status are more likely to be lost (positive to negative conversion) than gained (negative to positive conversion). Furthermore, conversion frequency varies significantly by the location of the metastasis, with ER discordance being statistically significantly higher in the central nervous system (CNS) and bone metastases compared with liver metastases.
Results
Summary of Results
The meta-analysis, pooling data from 39 studies on paired primary tumors and distant metastases, found the following random effects pooled percentages for discordance (total conversion):
-
Estrogen Receptor alpha (ERα): Total discordance was 19.3% (95% CI: 15.8% to 23.4%).
-
Positive to negative conversion: 22.5% (95% CI: 16.4% to 30.0%).
-
Negative to positive conversion: 21.5% (95% CI: 18.1% to 25.5%).
-
-
Progesterone Receptor (PR): Total discordance was 30.9% (95% CI: 26.6% to 35.6%).
-
Positive to negative conversion: 49.4% (95% CI: 40.5% to 58.2%). This occurred statistically significantly more often than negative to positive conversion (P < .001).
-
Negative to positive conversion: 15.9% (95% CI: 11.3% to 22.0%).
-
-
HER2: Total discordance was 10.3% (95% CI: 7.8% to 13.6%).
-
Positive to negative conversion: 21.3% (95% CI: 14.3% to 30.5%).
-
Negative to positive conversion: 9.5% (95% CI: 7.4% to 12.1%).
-
Location-Specific Discordance
The frequency of receptor conversion showed statistically significant differences based on the metastatic site, suggesting a location-specific pattern.
-
ERα Discordance:
-
Higher in CNS (20.8%) and bone (29.3%) metastases.
-
Lower in liver metastases (14.3%).
-
-
PR Discordance:
-
Higher in bone (42.7%) and liver (47.0%) metastases.
-
Lower in CNS metastases (23.3%).
-
-
HER2 Discordance: No statistically significant differences were observed between metastatic sites.
Assertive Critical Appraisal
Certainty of Evidence (GRADE Framework)
The certainty of evidence for the conversion percentages is generally Moderate due to the presence of substantial heterogeneity across the included studies.
Heterogeneity
High heterogeneity was reported for total ER conversion ($I^2 = 72.8\%$) and ER conversion from positive to negative ($I^2 = 78.3\%$). High heterogeneity ($I^2 = 77.0\%$) was also seen for PR conversion from positive to negative.
-
Definition: The $I^2$ statistic represents the percentage of variation across studies due to real differences in the conversion rates (e.g., patient population, assay method, or cancer characteristics) rather than just chance.
-
Implication: An $I^2$ of up to 78.3% indicates substantial heterogeneity, suggesting the studies are showing widely different results. The pooled average should therefore be interpreted with caution, as it represents a wide range of underlying values.
-
Mitigation: The authors performed subgroup analyses based on positivity thresholds (1% vs. 10% for ER/PR) and HER2 test type, which showed a decrease in heterogeneity in some subgroups, strengthening the validity of those more focused estimates.
Publication Bias
The authors did not assess for publication bias using formal methods, stating that a correct method to assess the amount of bias in diagnostic test accuracy meta-analyses is lacking. Publication bias is a common threat where studies with statistically significant or “positive” results are more likely to be published, which can lead to an overestimation of the true conversion rates in a meta-analysis.
Risk of Bias in Included Studies
The review performed a quality assessment of the 39 included studies using the QUADAS-2 tool (Quality Assessment of Diagnostic Accuracy Studies). This process led to the exclusion of several studies with high or unclear risk ratings, aiming to enhance the quality of the final quantitative synthesis (meta-analysis).
Reporting Quality Assessment (PRISMA)
The paper’s reporting quality adheres well to the PRISMA standard.
-
A PRISMA flow diagram (Figure 1) is included, clearly showing the study selection process from initial database records to the final 39 studies included in the quantitative synthesis.
-
The full search strategy for the Embase, Cochrane, and PubMed databases is described by listing the terms used.
Research Objective
The review’s question, framed by PICO:
-
P (Population): Patients with distant breast cancer metastases (excluding regional lymph nodes).
-
I (Index Test): Immunohistochemically (IHC) or in situ hybridization (ISH) assessed ERα, PR, and HER2 status in the distant metastasis.
-
C (Comparator/Reference Standard): IHC/ISH assessed ERα, PR, and HER2 status in the corresponding primary breast tumor.
-
O (Outcome): The frequency and direction of receptor conversion (discordance).
Study Design
The study is a Systematic Review and Meta-Analysis.
-
Search Strategy and Selection: Embase, Cochrane, and PubMed databases were searched from 1986 until July 2016. The search terms included “breast cancer” and “metastasis,” combined with “estrogen receptor,” “progesterone receptor,” “HER2/neu,” and “receptor conversion/discordance.”
-
Inclusion/Exclusion: Included original articles directly describing IHC-assessed ERα, PR, or HER2 status in primary breast tumors compared with paired distant metastases. Excluded were case reports, meta-analyses, reviews, cytology/fine needle aspirates, male patients, axillary lymph node/loco-regional metastases, and studies with fewer than 20 patients.
-
Statistical Analysis: A conservative random effects model was used to calculate the pooled percentages, which is appropriate for accounting for the observed high heterogeneity between studies.
Setting and Participants
-
Number of Studies: 39 studies were included in the quantitative synthesis (meta-analysis).
-
Number of Patients:
-
ERα discordance assessed in 1948 patients.
-
PR discordance assessed in 1730 patients.
-
HER2 discordance assessed in 2440 patients.
-
-
Characteristics: The mean age at primary diagnosis was 51 years. The mean time between primary tumor and matched distant metastasis was 51 months.
Bibliographic Data
-
Title: Receptor Conversion in Distant Breast Cancer Metastases: A Systematic Review and Meta-analysis
-
Authors: Willemijne A. M. E. Schrijver, Karijn P. M. Suijkerbuijk, Carla H. van Gils, Elsken van der Wall, Cathy B. Moelans, Paul J. van Diest
-
Journal: JNCI J Natl Cancer Inst
-
Year: 2018
- DOI: 10.1093/jnci/djx273
Fair Use & Copyright: This post provides a transformative, thesis‑driven critical appraisal intended for educational and scholarly purposes. It is not a reproduction of, nor a market substitute for, the original research article.
Support the Version of Record: To support the copyright holders and verify the underlying data—including primary survival curves, risk estimates, and other core outcomes—readers are strongly encouraged to access the original Version of Record via the link or DOI provided above.
Medical Disclaimer: This content is for informational and educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment.
