Comment:
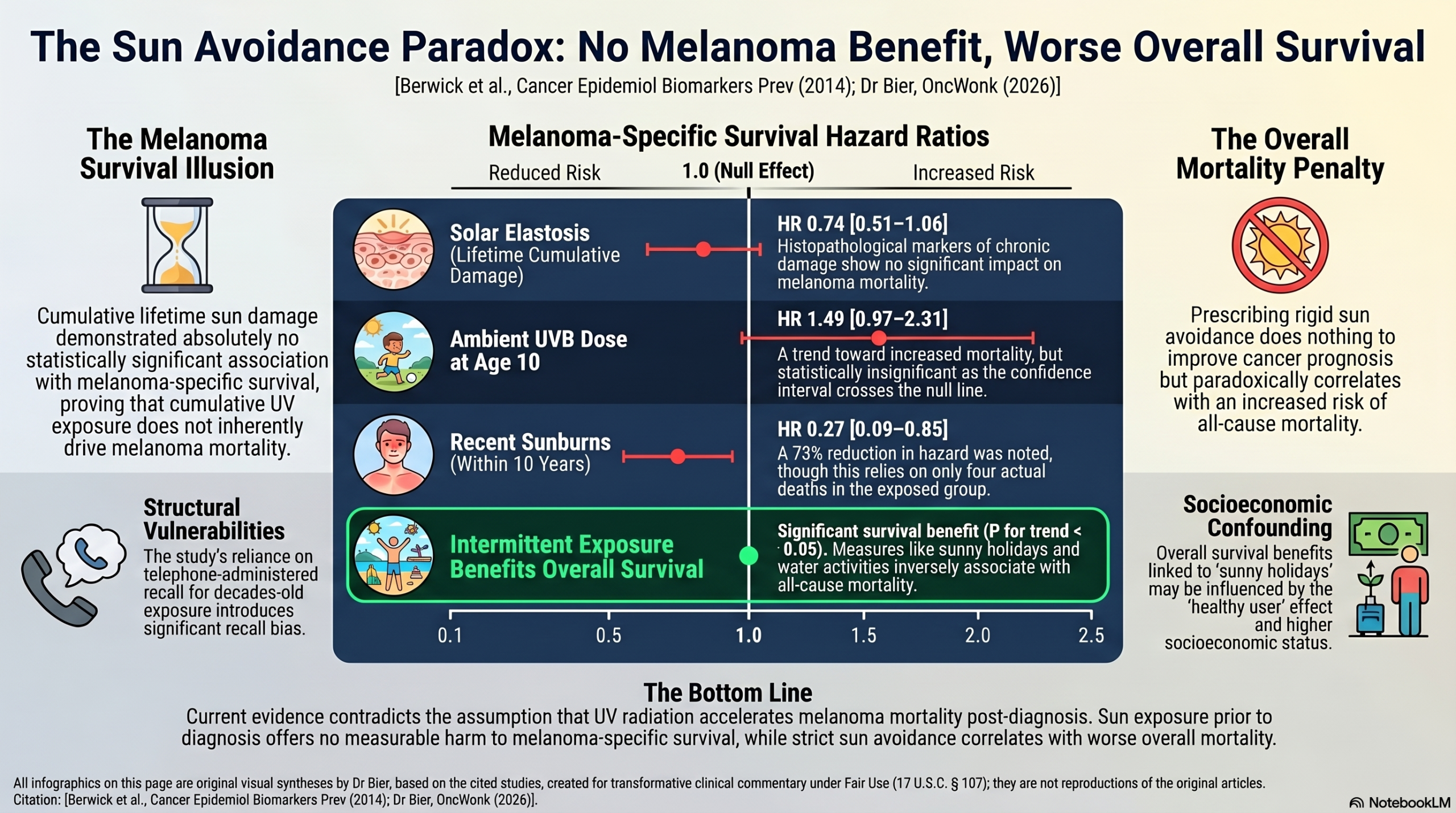
We stigmatize sun exposure despite numerous studies showing that it does not contribute to melanoma, and more importantly, increases overall survival. This study adds to data against the public health narrative that UV radiation drives melanoma mortality, showing that cumulative sun damage has no significant association with survival in people with melanoma. Solar elastosis—the gold-standard histopathological marker of lifetime sun damage—demonstrated no significant impact on melanoma-specific survival (HR = 0.74; 95% CI: 0.51–1.06).
The authors report a 49% increased risk of death associated specifically with UVB dose at age 10 (HR = 1.49), yet this was only significant as a p for trend with the confidence interval (0.97–2.31) crossing the null line. Because this was the only decade out of several tested to show a signal, it likely represents a statistical artifact of multiple testing rather than a true biological window of vulnerability as the comparison between the lowest and highest exposure groups was not significant. Even if it is accurate, then it only applies to children around that age group, and not to others. Another strange finding was that recent sunburns are “protective” (HR = 0.27) but that relied on only four deaths in the exposed group.
Most importantly, we should focus, as always, on overall survival. This study showed that while sun exposure had no impact on melanoma-specific death, it was significantly associated with improved overall survival. Avoiding the sun makes no improvement in melanoma related deaths, but increases overall deaths.
I am a strong advocate for the safety of sun exposure if done carefully, no different than exercise. The definitive takeaway from this study is a firm rejection of the idea that we can improve a patient’s prognosis by prescribing sun avoidance, which actually increases overall death rates.
The Wonk Debate – Audio Critique & Clinical Commentary:
Summary:
Clinical Bottom Line
This large, international observational study provides only weak evidence to support the hypothesis that sun exposure prior to a melanoma diagnosis improves melanoma-specific survival. While the authors previously suggested a protective effect in a smaller Connecticut-based study, these findings were largely not replicated here.
A notable finding is that any sunburn within 10 years of diagnosis was associated with a 73% reduction in the hazard of melanoma-specific death ; however, this result is based on a very small number of events (n=4) and should be interpreted with extreme caution. Furthermore, indicators of cumulative lifetime sun exposure, such as solar elastosis, showed no significant association with survival. Interestingly, while sun exposure had little impact on melanoma-specific death, it was associated with improved overall survival, which may reflect confounding by factors like socioeconomic status or a “healthy survivor” effect rather than a biological benefit of UV radiation on the tumor itself.
Results in Context
Main Results: Melanoma-Specific Survival
The study examined various measures of ultraviolet radiation (UVR) exposure and their relationship to death specifically caused by melanoma:
- Recent Sunburns: Having at least one painful/blistered sunburn in a year within the decade prior to diagnosis was inversely associated with melanoma mortality (Fully adjusted HR 0.27, 95% CI 0.09–0.85, P=0.03).
- Lifetime Cumulative Exposure: Histological solar elastosis (a marker of long-term skin damage) was not significantly associated with survival (HR 0.74, 95% CI 0.51–1.06, P=0.10).
- Intermittent Exposure: Neither holiday sun hours nor water-related outdoor activities within 10 years of diagnosis showed a significant association with melanoma-specific survival.
- Early Life Exposure: High ambient UVB dose at age 10 was actually associated with a trend toward increased melanoma mortality (Fully adjusted HR 1.49, 95% CI 0.97–2.31 for the highest vs. lowest quartile, P=0.03).
Overall Survival vs. Cancer-Specific Survival
The study found a discrepancy when looking at all-cause mortality:
- Measures of intermittent sun exposure (UVB dose, holiday sun, water activities) were significantly and inversely associated with overall survival (P for trend <0.05 for most).
- The authors suggest that while sun exposure might appear to impact overall survival, the study was not designed to evaluate non-melanoma deaths, and these findings could be confounded by lifestyle or socioeconomic status.
Clinical and Host Factors
Traditional prognostic factors remained strongly associated with survival:
- Breslow Thickness: Patients with lesions >4.00 mm had a 13.8 times higher hazard of death compared to those with lesions <1.00 mm.
- Sex: Women had a lower risk of dying from melanoma than men (HR 0.56, P=0.0002).
- Education: Higher education levels were associated with a reduced hazard of death (HR 0.69, P=0.03).
Definitions
- Hazard Ratio (HR): A measure of how often a particular event (death) happens in one group compared to another over time. An HR of 0.27 means the group had 73% lower hazard of the event during the study period.
- Solar Elastosis: The accumulation of abnormal elastin in the dermis, serving as an objective histopathological marker of chronic, cumulative sun damage.
Assertive Critical Appraisal
Limitations & Bias (STROBE Framework)
- Small Event Size for Key Finding: The “protective” association of recent sunburns is the study’s most provocative finding, yet it relied on only four deaths in the sunburn-exposed group. This leads to extreme imprecision and a high risk of a “Type I” error (finding a significance that isn’t truly there).
- Recall Bias: Sun exposure data was collected via telephone interviews, requiring patients to recall habits from decades prior. Patients with a cancer diagnosis may recall their sun exposure differently than those without, potentially biasing the results.
- Confounding: While the authors adjusted for education, socioeconomic status remains a major potential confounder for “sunny holidays” and “water activities”. These activities are often markers of higher wealth, which is independently associated with better healthcare access and survival.
Reporting Quality Assessment (STROBE)
The study quality is high regarding its recruitment and description of the population. The authors clearly described their efforts to address confounding by including age, sex, education, and anatomic site in their “fully adjusted” models. However, the use of death certificates for cause-of-death verification is a noted limitation, as metastases can sometimes be misclassified (e.g., melanoma lung mets labeled as primary lung cancer), which would reduce statistical power.
Applicability
The findings are highly generalizable due to the multi-center, international design covering diverse latitudes (Australia, USA, Canada, Italy). However, for a clinician, the primary takeaway is that while sun exposure is a well-established risk factor for melanoma incidence , there is no reliable evidence to suggest that “prescribing” sun exposure or relaxing sun-safety habits will improve the prognosis of a patient once they are diagnosed.
Research Objective
To evaluate the hypothesis that sun exposure prior to a melanoma diagnosis is associated with improved melanoma-specific survival in a large, international population.
Study Design
A multi-center, international population-based observational study.
- Participants: 3,578 incident melanoma cases (2,372 single primary; 1,206 multiple primary).
- Follow-up: Average of 7.4 years.
- Analysis: Cox proportional hazards models were used to calculate HRs, adjusting for potential confounders like age, sex, and tumor site.
Setting and Participants
- Locations: Australia (New South Wales, Tasmania), Italy (Piedmont), Canada (British Columbia, Ontario), and the USA (New Jersey, North Carolina, California, Michigan).
- Inclusion: Patients diagnosed with incident first or multiple primary melanomas between 1998 and 2003.
- Participation Rate: 54% for those completing all aspects including DNA sampling.
Bibliographic Data
- Title: Sun Exposure and Melanoma Survival: A GEM Study
- Authors: Berwick M, Reiner AS, Paine S, et al.
- Journal: Cancer Epidemiology, Biomarkers & Prevention
- Year: 2014
- DOI: 10.1158/1055-9965.EPI-14-0431
Fair Use & Copyright: This post provides a transformative, thesis‑driven critical appraisal intended for educational and scholarly purposes. It is not a reproduction of, nor a market substitute for, the original research article.
Support the Version of Record: To support the copyright holders and verify the underlying data—including primary survival curves, risk estimates, and other core outcomes—readers are strongly encouraged to access the original Version of Record via the link or DOI provided above.
Medical Disclaimer: This content is for informational and educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment.
