Comment:
This synthesis of 80 meta-analyses corrects the long-standing bias that favors high-intensity aerobic training over more accessible, multi-systemic interventions. While aerobic fitness remains a vital component of recovery, this review highlights that Tai Chi and Qigong are clinically efficacious for preserving functional independence and psychological resilience. These modalities offer high-value interventions for addressing treatment-related toxicities—including sleep quality, social well-being, and upper-body strength—with a safety profile that acknowledges the physiological fragility of patients in active treatment. The definitive takeaway is that a diversified exercise prescription, which includes mind-body practices, is a requirement for maintaining the physical and psychological infrastructure necessary for long-term survival.
The Wonk Debate – Audio Critique & Clinical Commentary:
Summary:
Clinical Bottom Line
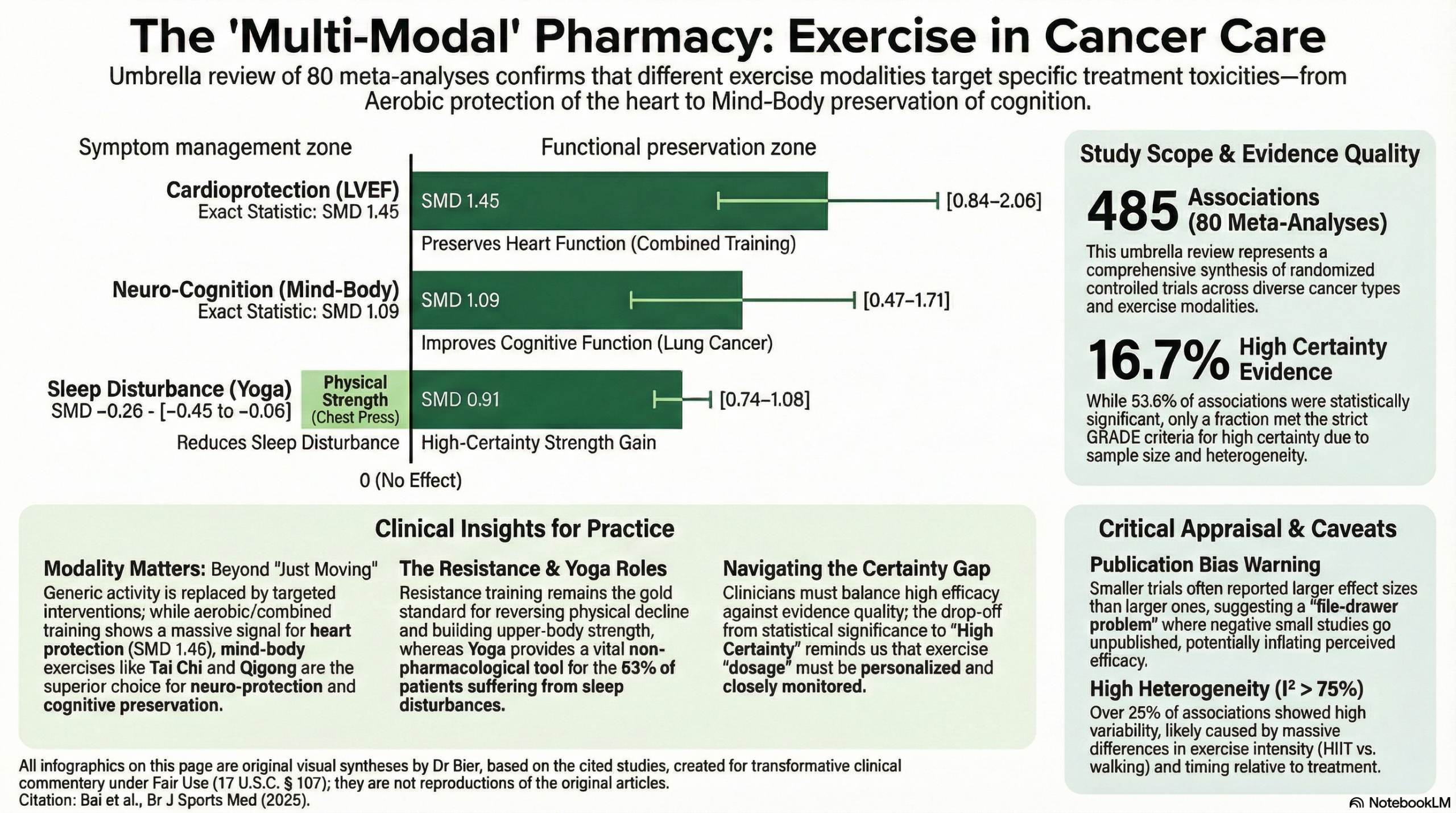
This high-level umbrella review provides robust evidence that exercise is a multi-system “medicine” for cancer patients, significantly reducing treatment-related toxicities (such as cardiotoxicity and neuropathy) while enhancing psychological well-being and physical function. While 53.6% of identified associations were statistically significant, clinicians should note that only 16.7% reached “high-certainty” evidence under GRADE criteria. Exercise—including aerobic, resistance, and mind-body practices—should be viewed as a standard adjuvant component of cancer care to mitigate adverse events and improve overall quality of life.
Results
- Summary of Results: The review synthesized 485 associations from 80 meta-analyses. High-certainty evidence supports exercise for:
- Physical Function: Improvement in VO2peak , aerobic fitness , and muscular strength (chest/leg press) in breast cancer (BC).
- Symptom Management: Reduction in cancer-related fatigue (via HIIT or walking+resistance) and improvement in sleep quality.
- Quality of Life (QoL): Enhanced HRQoL in BC and colorectal cancer (CRC).
- Psychological Health: Reduction in anxiety (via Qigong/Tai Chi).
- Definitions: * Standardised Mean Difference (SMD): A statistical measure used to combine results from studies using different scales; 0.2 is small, 0.5 is medium, and 0.8 is large.
- Relative Risk (RR): The ratio of the probability of an outcome in an exposed group to the probability of an outcome in an unexposed group.
Assertive Critical Appraisal
- Certainty of Evidence (GRADE Framework): Only 81 (16.7%) associations were rated as High Certainty. Reasons for downgrading the remaining evidence included:
- Imprecision: Many meta-analyses included fewer than five primary studies, leading to small total populations (N < 400 for continuous variables).
- Heterogeneity: High variability in exercise parameters (intensity, duration) and cancer types contributed to inconsistent findings.
- Heterogeneity: The I2 statistic showed that 25.4% of associations had high heterogeneity (I2 > 75%). This indicates the studies showed widely different results, likely due to variations in exercise “dosing” and timing (during vs. after treatment).
- Publication Bias: The authors noted that smaller and medium-sized trials often exhibited greater treatment effects than the largest trials, suggesting potential publication bias where negative small studies may go unpublished.
- Risk of Bias in Included Studies: Methodological quality was generally strong, with 82.5% of the meta-analyses rated as High Quality via AMSTAR.
- Special Consideration for Pooled Results: While many pooled results reached significance, the authors caution that results for some outcomes (e.g., cognitive function, specific biomarkers) were driven by a small number of underpowered studies, requiring more large-scale RCTs to confirm benefits.
- Reporting Quality Assessment (PRISMA): The study strictly adhered to PRISMA guidelines and included a clear flow diagram showing the selection process from 3,070 identified records down to the final 80 studies.
Research Objective
- Population: Individuals diagnosed with any type of cancer.
- Intervention: Any form of exercise (Aerobic, Resistance, HIIT, Yoga, Tai Chi, Qigong).
- Comparison: Usual care or no exercise.
- Outcome: Comprehensive health outcomes (adverse effects, body composition, psychological status, social function) .
Study Design
- Type: Umbrella review (systematic review of systematic reviews/meta-analyses).
- Databases: PubMed, Embase, Cochrane, and Web of Science searched up to July 23, 2024.
- Inclusion: Meta-analyses of RCTs only.
Setting and Participants
- Total Studies: 80 meta-analyses.
- Total Associations: 485 unique health associations.
- Cancer Types: Predominantly breast cancer (50.3%), followed by lung (9.7%), digestive (4.1%), and hematological (2.7%).
Bibliographic Data
- Title: Impact of exercise on health outcomes in people with cancer: an umbrella review of systematic reviews and meta-analyses of randomised controlled trials
- Authors: Xue-Li Bai, Yu Li, Zan-Fei Feng, Fan Cao, Dong-Dong Wang, Jing Ma, et al.
- Journal: British Journal of Sports Medicine (Br J Sports Med)
- Year: 2025
- DOI: 10.1136/bjsports-2024-109392
Fair Use & Copyright: This post provides a transformative, thesis‑driven critical appraisal intended for educational and scholarly purposes. It is not a reproduction of, nor a market substitute for, the original research article.
Support the Version of Record: To support the copyright holders and verify the underlying data—including primary survival curves, risk estimates, and other core outcomes—readers are strongly encouraged to access the original Version of Record via the link or DOI provided above.
Medical Disclaimer: This content is for informational and educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment.
