Comment:
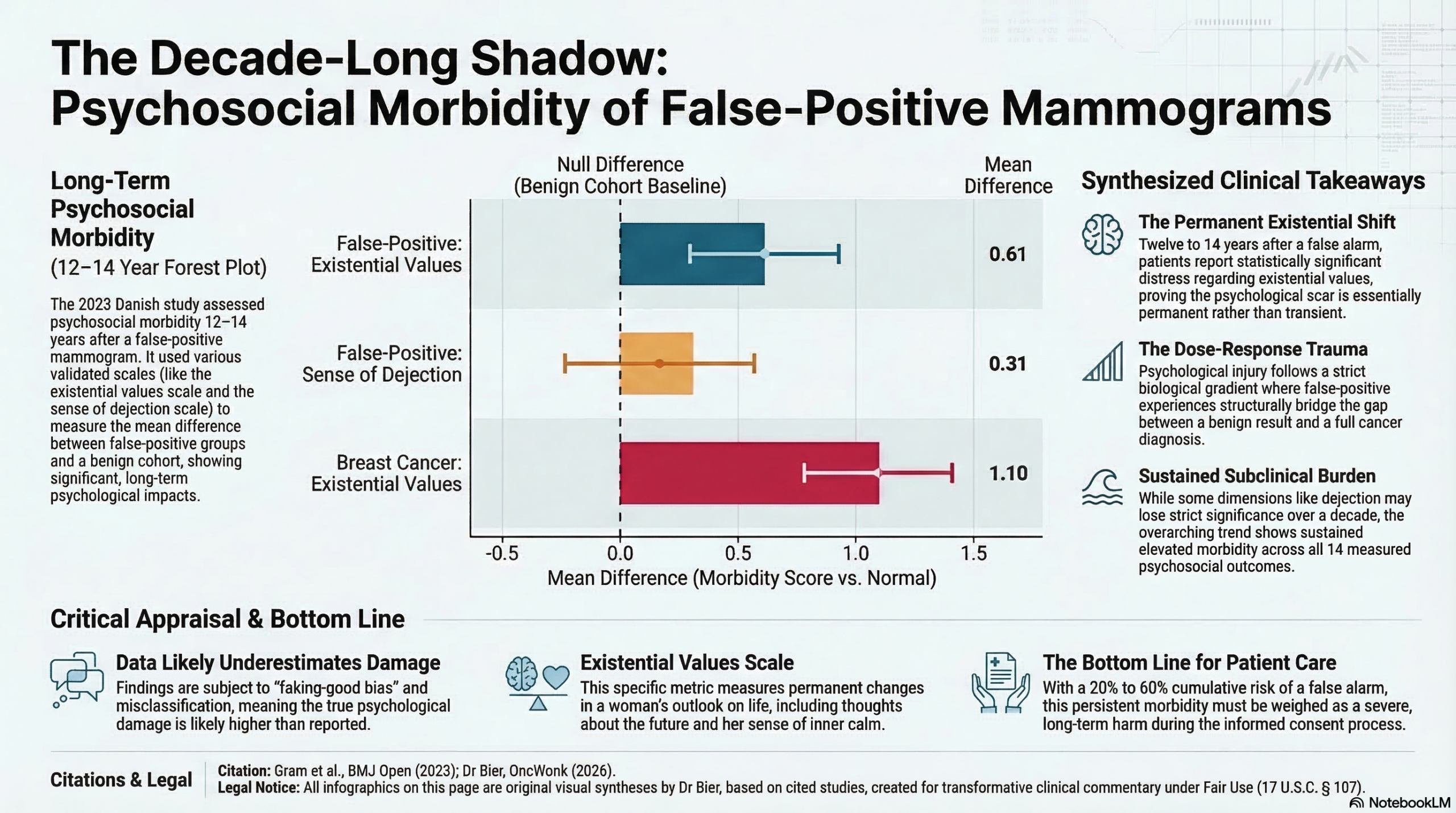
There are multiple studies in the literature showing lasting psychological damage from a false positive mammogram requiring a follow-up to establish that it’s benign, but this one is notable for the longest follow-up period. For those advocating screening, the reality is that the resulting false alarms inflict decade-long psychological damage. Knowing that 20% to 60% of women will experience a false positive over a decade of screening, the findings here are staggering. Twelve to 14 years after their false alarm, these women still reported elevated distress across all 14 measured outcomes compared to women with normal results, with a statistically significant, permanent alteration to their existential values (Mean difference 0.61).
We have to acknowledge that subjecting a healthy population to the existential terror of a lethal disease does not resolve with a negative biopsy; it permanently shifts how they view their health and future.
The Wonk Debate – Audio Critique & Clinical Commentary:
Summary:
Clinical Bottom Line
This matched cohort study provides evidence that the psychosocial harms of a false-positive mammogram persist for over a decade. While the intensity of these consequences diminishes over time, women with false-positive results still report higher psychosocial distress 12–14 years later compared to women with normal findings, particularly regarding existential values. Clinicians should recognize that a “false alarm” in breast cancer screening is not a transient event for many women; these findings should be integrated into shared decision-making and informed consent processes prior to screening.
Results in Context
Main Results
The study utilized the Consequences Of Screening-Breast Cancer (COS-BC) questionnaire, which measures 14 psychosocial dimensions.
- False-Positive vs. Normal: Women with false-positive results reported higher psychosocial consequences across all 14 outcomes compared to those with normal results.
- Statistical Significance: Most mean differences moved toward the null over time, but the existential values scale remained significantly affected 12–14 years later (Mean difference: 0.61; 95% CI 0.15 to 1.06; p=0.009).
- Definitions: A false-positive result occurs when an initial abnormal screening mammogram is later confirmed to be non-malignant through further testing (e.g., imaging or biopsy). The existential values scale measures changes in a woman’s outlook on life, such as thoughts about the future and sense of inner calm.
Participants
- Initial Cohort (2004-2005): Approximately 30,000 women screened.
- Baseline Participants: 454 with abnormal results (174 breast cancer, 272 false-positive) and 908 matched controls with normal results.
- Final Follow-up (12-14 years): 761 women (65% of survivors) completed the questionnaire, including 156 in the false-positive group and 520 in the normal group.
Assertive Critical Appraisal
Limitations & Bias (STROBE Framework)
- Classification Bias: Screening results were only assessed at baseline. Because women in the “normal” group likely underwent subsequent screenings over the 14-year period, some may have received false-positive results later, which would underestimate the true difference between groups.
- Attrition Bias: There was differential non-response; women with lower socioeconomic status or greater psychosocial distress were more likely to drop out. However, the authors appropriately used Inverse Probability Weighting (IPW) to adjust for this attrition.
- Faking-Good Bias: Qualitative interviews within this cohort suggested women might underreport distress because they are “eager to disprove” that screening causes harm, potentially biasing results toward the null.
Reporting Quality Assessment (STROBE)
- Confounding: The authors clearly described efforts to address confounding, adjusting for age, cohabitation, employment, and socioeconomic status.
- Dose-Response Association: A major strength is the inclusion of a “breast cancer” benchmark. The data showed a “psychological gradient” where women with breast cancer were most affected, followed by false-positives, and then normal results. This biological gradient supports a causal link between the screening result and the long-term psychosocial impact.
Applicability
The findings are highly relevant to general practice, especially given that the cumulative risk of a false-positive result over 10 years of screening is estimated between 20% and 60%. While conducted in Denmark’s public healthcare system, the psychological impact of a cancer scare is likely universal, though cultural nuances in “welfare states” may influence specific coping mechanisms.
Research Objective
To compare the psychosocial consequences of mammography screening among women with breast cancer, normal results, and false-positive results over a long-term follow-up of 12–14 years.
Study Design
A matched cohort study with assessments at six time points: baseline, 1, 6, 18, 36 months, and 12–14 years.
Setting and Participants
- Setting: Two Danish screening centers (2004–2019).
- Participants: Women aged 50–69 years invited to biennial mammography screening.
Bibliographic Data
- Title: Long-term psychosocial consequences of false-positive screening mammography: a cohort study with follow-up of 12–14 years in Denmark
- Authors: Emma Grundtvig Gram, Volkert Siersma, John Brandt Brodersen
- Journal: BMJ Open
- Year: 2023
- DOI: 10.1136/bmjopen-2023-072188
Original Article:
Full text: PubMed Central
Fair Use & Copyright: This post provides a transformative, thesis‑driven critical appraisal intended for educational and scholarly purposes. It is not a reproduction of, nor a market substitute for, the original research article.
Support the Version of Record: To support the copyright holders and verify the underlying data—including primary survival curves, risk estimates, and other core outcomes—readers are strongly encouraged to access the original Version of Record via the link or DOI provided above.
Medical Disclaimer: This content is for informational and educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment.
